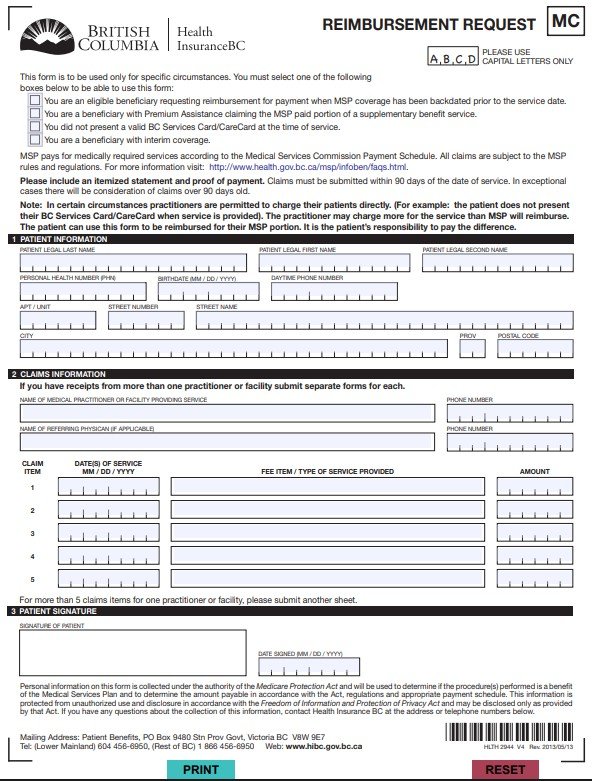
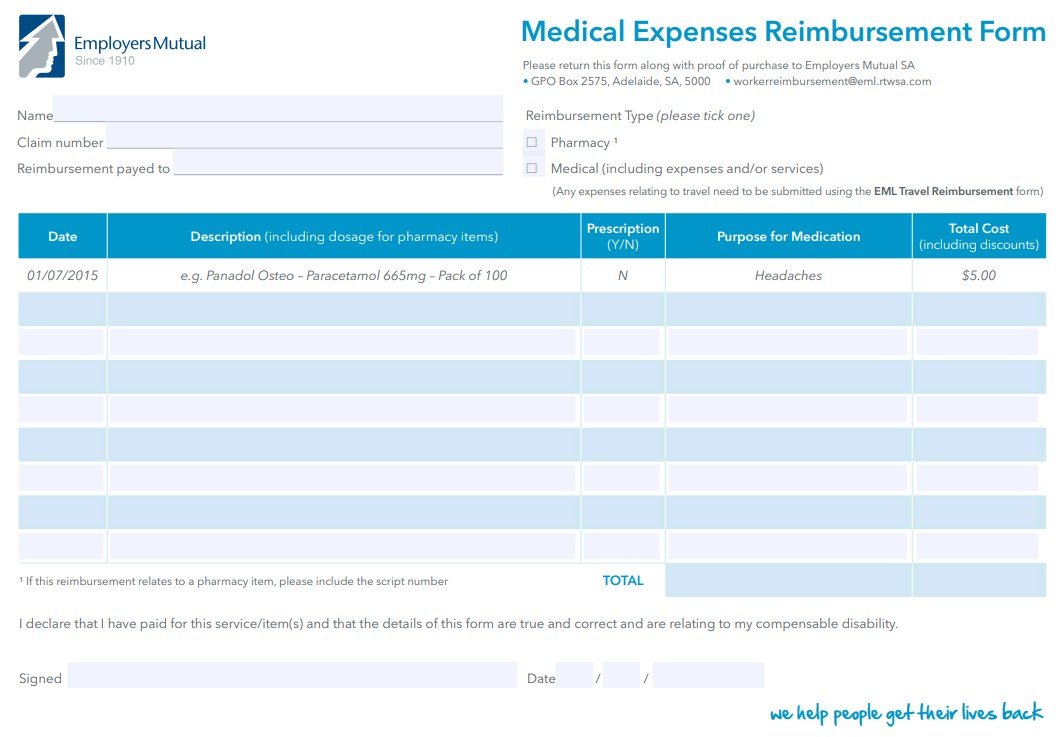
A medical reimbursement form is a document you submit to your employer, insurance company, or healthcare program to claim back money you’ve already spent on medical treatment.
This usually applies in situations like:
- Visiting a doctor not in your insurance network
- Paying upfront for emergency treatment
- Buying medicines from a pharmacy
- Getting diagnostic tests done privately
Navigating healthcare costs is often stressful for many families. When you pay upfront for doctor visits or hospital stays, getting your cash back becomes a top priority. Understanding your coverage is the first step toward achieving financial peace.
Accuracy is vital to avoiding denials and ensuring a smooth payout experience. A properly filled medical claim form bridges the gap between your expensive bills and the insurance company. A tiny mistake can lead to long delays or even a rejected request.
This guide simplifies the reimbursement process to help you secure every dollar you deserve. We will walk through the steps of gathering detailed receipts and tracking your digital request. Our goal is to make the paperwork feel much less intimidating.
Taking control of your healthcare finances feels truly empowering. Let’s explore how to handle these essential documents with total confidence and ease today. Following the right steps ensures you get your money back faster.
Table of Contents
Key Takeaways
- Verify your specific insurance policy coverage before filing.
- Collect detailed itemized statements from all your providers.
- Confirm the correct mailing address or digital submission portal.
- Review all entry fields for typos or missing personal data.
- Note down the exact date you submitted your request.
- Follow up with your carrier if processing delays occur.
- Save a digital scan of every paper you submit.
Understanding the Basics of Medical Reimbursement
When it comes to managing medical expenses, understanding the reimbursement process is key to financial planning. Medical reimbursement is a process where individuals can claim back the money they spent on medical expenses from their insurance providers.
What is a Medical Reimbursement Form
A medical reimbursement form is a document that individuals need to fill out to initiate the reimbursement process. This form typically requires personal and policy information, details of the medical services received, and the total amount being claimed.
Filling out this form accurately is crucial for a smooth reimbursement process. It serves as a formal request to the insurance provider to review the claim and reimburse the expenses incurred.
Why You Need to File for Reimbursement
Filing for reimbursement is essential for recovering the costs of medical treatments and services. Without filing a claim, individuals may not receive the financial compensation they are entitled to under their insurance policy.
The reimbursement process helps in reducing the financial burden of medical expenses, making healthcare more affordable. It’s a vital step in managing healthcare costs effectively.
Common Scenarios Requiring a Claim
There are several scenarios where filing a medical reimbursement claim is necessary. These include:
- Out-of-pocket expenses for doctor visits and treatments
- Prescription medication costs
- Hospital stays and surgical procedures
- Diagnostic tests and procedures
Here’s a simple breakdown of common medical services and their typical reimbursement status:
| Medical Service | Typical Reimbursement Status |
|---|---|
| Doctor Visits | Generally Reimbursable |
| Prescription Medication | Often Reimbursable with Proper Documentation |
| Hospital Stays | Usually Reimbursable |
Preparing Your Documentation Before You Start
To ensure a smooth claim submission, preparing your documentation is a crucial first step. Before you begin the medical reimbursement process, it’s vital to have all necessary documents in order. This preparation will not only save you time but also reduce the likelihood of delays or rejections due to incomplete information.
Gathering Itemized Medical Bills
The first step in preparing your documentation is to gather itemized medical bills for the services you’ve received. These bills should detail the specific treatments, procedures, or services provided, along with their corresponding costs. It’s essential to ensure that these bills are itemized, as lump sum bills may not provide enough detail for your insurance provider to process your claim.
Key elements to look for in an itemized bill include:
- Date of service
- Description of the service or procedure
- Charge for each service
Collecting Proof of Payment
In addition to itemized bills, you’ll need to collect proof of payment for the medical expenses you’re claiming. This can include receipts, credit card statements, or bank statements showing the payment for medical services. Ensuring you have this documentation will help verify that you’ve paid for the services you’re claiming.
Examples of acceptable proof of payment:
| Document Type | Description |
|---|---|
| Receipts | Detailed receipts showing the amount paid |
| Credit Card Statements | Statements highlighting the transaction related to medical expenses |
| Bank Statements | Statements showing the payment for medical services |
Organizing Your Explanation of Benefits
The Explanation of Benefits (EOB) is a statement from your insurance provider that explains how your claim was processed. It’s crucial to organize your EOBs as they provide essential information about what was covered, what wasn’t, and any amount you’re responsible for paying. Ensuring you have these documents organized will help you understand your coverage and facilitate the reimbursement process.
“The EOB is not a bill, but rather an explanation of how your claim was processed. It will detail the services covered, the amount paid, and any remaining balance you’re responsible for.”
By gathering itemized medical bills, collecting proof of payment, and organizing your Explanation of Benefits, you’ll be well-prepared to move forward with your medical reimbursement claim. This preparation is key to ensuring a smooth and efficient process.
Navigating Your Insurance Provider Portal
Insurance providers often offer online portals to simplify the claim submission process, making it easier for policyholders to file for medical reimbursement. These portals are designed to streamline the process, reducing the time and effort required to submit a claim.
Creating an Online Account
The first step in navigating your insurance provider’s portal is creating an online account. This typically involves visiting the insurance company’s website and locating the registration or sign-up section. You will be required to provide some personal and policy details to verify your identity.
Key Information Required for Account Creation:
- Policy number
- Date of birth
- Email address
- Password creation
Locating the Correct Claim Submission Page
Once you have successfully logged in, you need to find the claim submission page. This is usually found under sections labeled “Claims,” “Submit a Claim,” or “Reimbursement Requests.” Insurance portals may vary in design, but most have a straightforward process for locating this page.
Downloading the Official Medical Reimbursement Form
After locating the claim submission page, you will typically find a link to download the official medical reimbursement form. It’s crucial to use this form to ensure that your claim is processed correctly. The form may be available in PDF or another format.
Here’s a comparison of the key features of online claim submission portals offered by some major insurance providers in the United States:
| Insurance Provider | Online Portal Availability | Claim Submission Process |
|---|---|---|
| Blue Cross Blue Shield | Yes | Direct online submission |
| Aetna | Yes | Online submission with optional upload |
| Cigna | Yes | Online submission with required documentation upload |
By understanding how to navigate your insurance provider’s online portal, you can efficiently submit your medical reimbursement claims and track their status.
Step-by-Step Guide to Filling Out Your Medical Reimbursement Form
To ensure a smooth reimbursement process, it’s essential to accurately fill out your medical claim form. This guide will walk you through the necessary steps to complete the form correctly, ensuring that your claim is processed without unnecessary delays.
Providing Personal and Policy Information
The first section of the medical reimbursement form requires you to provide personal and policy information. This includes your name, policy number, and contact details. Ensure that all information is accurate and matches the details on your insurance policy.
- Full name as it appears on the insurance policy
- Policy number and any other relevant policy identifiers
- Contact information, including phone number and email address
Detailing the Medical Services Received
When detailing the medical services received, it’s crucial to be thorough and precise. You will need to provide the date of service, a description of the service, and the amount charged.
- Date of service: The date when you received the medical treatment.
- Description of service: A clear and concise description of the medical service provided.
- Amount charged: The total amount billed by the healthcare provider for the service.
Calculating the Total Amount Requested
After detailing all the medical services received, you need to calculate the total amount you are requesting for reimbursement. Ensure that you have all the necessary receipts and bills to support the amount claimed.
Tips for accurate calculation:
- Sum up all the amounts charged for the services received.
- Ensure you have itemized bills to support your claim.
- Double-check your calculations to avoid errors.
Verifying Provider Information and Tax IDs
It’s also important to verify the information of the healthcare provider, including their name, address, and Tax ID number. This information is crucial for the insurance company to process your claim correctly.
To verify provider information:
- Check your medical bills or receipts for the provider’s details.
- Ensure the Tax ID number is correctly provided to avoid any processing issues.
By following these steps and ensuring that all information is accurate and complete, you can facilitate a smooth and efficient reimbursement process for your medical expenses.
Common Mistakes to Avoid When Filing Claims
Missing Signatures and Dates
Submitting Illegible Receipts
Incorrect Coding or Procedure Descriptions
Failing to Include Necessary Attachments
| Common Mistakes | Consequences | Prevention Tips |
|---|---|---|
| Missing Signatures and Dates | Immediate rejection or requests for additional information | Double-check all documents for signatures and dates |
| Submitting Illegible Receipts | Delays in claim processing | Ensure all documents are clear and legible; obtain duplicates if necessary |
| Incorrect Coding or Procedure Descriptions | Denials or underpayment of claims | Verify codes match the services described in supporting documentation |
| Failing to Include Necessary Attachments | Delays or denial of claims | Use a checklist to ensure all necessary documents are attached |
Submitting Your Claim Electronically Versus by Mail
Understanding the best method for submitting your medical reimbursement form is crucial for a hassle-free reimbursement process. Both electronic and mail submissions have their advantages, and the choice between them depends on several factors.
Benefits of Online Submission Portals
Submitting your claim electronically offers several benefits, including faster processing times and reduced paperwork. Online portals allow you to upload your documents directly, minimizing the risk of lost or misplaced paperwork. Moreover, electronic submissions often come with automated acknowledgments, ensuring that your claim has been received by the insurance provider.
Faster Processing: Electronic claims are typically processed quicker than their mailed counterparts, as they are received and reviewed more promptly.
Convenience: Online portals are accessible 24/7, allowing you to submit your claim at a time that suits you best.
When to Use Traditional Mail Services
While electronic submission is generally preferred for its speed and efficiency, there are scenarios where traditional mail services are more appropriate. For instance, if you are uncomfortable with digital submissions or lack access to the necessary technology, mailing your claim is a viable alternative.
Additionally, certain documents may be required to be submitted in their original form, making mail the only suitable option. It’s also worth noting that some insurance providers may still require certain claims to be mailed, so it’s essential to check with your provider.
Tracking Your Submission Status
Regardless of the submission method you choose, tracking the status of your claim is vital. For electronic submissions, most online portals offer a tracking feature that allows you to monitor the progress of your claim. If you’ve chosen to mail your claim, consider using a trackable mail service to ensure it reaches its destination.
Following up with your insurance provider can also provide insights into the status of your claim. Keeping a record of your submission, including the date and method of submission, can be helpful in case of any discrepancies or delays.
Understanding Timelines and Processing Expectations
Understanding the timeline for processing insurance claims can help manage expectations and reduce anxiety for those awaiting reimbursement.
Typical Turnaround Times for Claims
The time it takes for an insurance claim to be processed can vary significantly depending on several factors, including the complexity of the claim and the efficiency of the insurance provider’s processing system.
Generally, straightforward claims with all necessary documentation can be processed within a few days to a couple of weeks. However, more complex claims may take longer, sometimes requiring several weeks or even months to resolve.
What Happens During the Review Process
During the review process, the insurance company evaluates the claim to determine its validity and the extent of the coverage. This involves verifying the information provided, checking the policy details, and assessing the medical services received against the policy’s coverage terms.
The review process may also involve requesting additional information if the initial submission is incomplete or if further clarification is needed on certain aspects of the claim.
Handling Requests for Additional Information
If the insurance company requests additional information, it’s essential to respond promptly to avoid delays in the processing of your claim.
To handle such requests efficiently:
- Keep all relevant documents readily available.
- Respond to the request as soon as possible.
- Ensure that the information provided is accurate and complete.
By doing so, you can help expedite the review process and move closer to receiving your reimbursement.
What to Do If Your Claim Is Denied
If your medical claim is denied, it’s essential to know how to respond effectively to potentially overturn the decision. A denied claim can be disappointing, but understanding the reasons behind it and the subsequent steps can help you navigate the situation more effectively.
Reviewing the Explanation of Benefits
The first step after receiving a denied claim is to carefully review the Explanation of Benefits (EOB) statement provided by your insurance company. The EOB will detail the reasons for the denial, which could range from incorrect coding to services not covered under your policy.
It’s crucial to verify that the information on the EOB matches your medical claim form and the services you received. Any discrepancies should be noted and addressed in your next steps.
Understanding the Appeals Process
If you believe your claim was denied in error, you have the right to appeal the decision. The EOB will typically include information on how to initiate the reimbursement process appeal, including any deadlines and required documentation.
It’s essential to follow the instructions provided carefully and to submit any additional information that supports your claim. This might include further documentation from your healthcare provider or a detailed letter explaining why you believe the denial was incorrect.
Gathering Supporting Evidence for a Re-evaluation
Gathering supporting evidence is a critical step in the appeals process. This can include medical records, receipts, and any other relevant documentation that supports your claim. Ensure that all documents are accurate, complete, and clearly legible.
Organizing your evidence in a clear and concise manner will help facilitate the review process. Consider creating a cover letter that outlines your appeal and references the supporting documents you’ve included.
By understanding the appeals process and preparing your case thoroughly, you can effectively challenge a denied claim and potentially achieve a more favorable outcome in your reimbursement process.
Tips for Faster Reimbursement Success
To expedite your medical reimbursement, consider implementing a few strategic practices that can make a significant difference in the processing time and overall success of your claim.
Keeping Digital Copies of All Records
Maintaining digital copies of your medical bills, receipts, and insurance documents can greatly streamline the reimbursement process.
- Scan or photograph your medical bills and receipts for digital storage.
- Organize your digital files in a dedicated folder with clear labels.
- Consider using cloud storage services for secure and accessible document management.
Double-Checking Forms Before Submission
One of the most critical steps in ensuring a smooth reimbursement process is to thoroughly review your claim forms before submission.
Key areas to focus on:
- Verify that all personal and policy information is accurate and up-to-date.
- Ensure that the medical services detailed are correct and supported by the attached documentation.
- Confirm that the total amount requested is calculated correctly.
Communicating Effectively with Insurance Representatives
Effective communication with your insurance representatives is crucial for resolving any issues that may arise during the reimbursement process.
Tips for effective communication:
- Have all relevant documents and information readily available.
- Clearly state the purpose of your call or message.
- Take notes during the conversation, including the representative’s name and any agreed-upon next steps.
Conclusion
Accurately completing a medical reimbursement form is crucial for a smooth claim submission process. By understanding the basics of medical reimbursement and preparing the necessary documentation, you can ensure a seamless experience.
Filing a claim requires attention to detail, from providing personal and policy information to detailing the medical services received. Avoiding common mistakes, such as missing signatures and incorrect coding, can significantly reduce the risk of claim denial.
Submitting your claim electronically or by mail requires careful consideration. Understanding the typical turnaround times and processing expectations can help you plan and follow up on your claim.
By following the steps outlined in this article and maintaining a record of your submissions, you can ensure a successful medical reimbursement experience. Effective communication with your insurance provider is key to resolving any issues that may arise during the claim submission process.
With the knowledge gained from this article, you are now well-equipped to handle your medical reimbursement claims with confidence, ensuring that you receive the reimbursement you are entitled to.
medical reimbursement form
medical expenses reimbursement form
medical charges reimbursement form
medical bill reimbursement form
insurance reimbursement form
FAQs:
What exactly is a medical reimbursement form and when should I use it?
A medical reimbursement form is an official document used to request repayment from your insurance provider, such as UnitedHealthcare or Aetna, for healthcare costs you paid out-of-pocket. You typically need to file this when you receive care from an out-of-network provider or if a provider is unable to file a claim on your behalf at the time of service.
What specific documentation do I need to gather before submitting my claim?
To ensure a smooth process, you should have your itemized medical bills (often referred to as a Superbill), proof of payment (such as a receipt or bank statement), and your insurance Member ID card. It is also helpful to have your most recent Explanation of Benefits (EOB) handy to track your deductible and out-of-pocket maximum progress.
Why does the insurance company require the Provider’s Tax ID and NPI number?
Insurers like Cigna and Blue Cross Blue Shield use the Tax ID and National Provider Identifier (NPI) to verify the legitimacy of the healthcare professional or facility. These numbers are essential for the insurance company to categorize the claim correctly and prevent fraudulent submissions.
Can I submit my medical reimbursement form through an online portal?
Yes! Most modern carriers, including Kaiser Permanente and Humana, encourage using their online member portals or mobile apps. Submitting electronically is usually much faster than traditional mail and allows you to receive real-time status updates on your claim’s progress.
What are the most common mistakes that lead to a claim being denied?
The most frequent errors include missing signatures, illegible receipts, and incorrect CPT (Current Procedural Terminology) codes. Additionally, failing to include the ICD-10 diagnosis codes can lead to a denial because the insurance company cannot verify the medical necessity of the procedure.
How long does it typically take for an insurance company to process a reimbursement?
While timelines vary by provider, most major insurers like Anthem aim to process “clean claims” within 30 days. If you submit your documentation via the USPS, you should allow extra time for mail transit. Electronic submissions are often settled significantly faster.
What should I do if my reimbursement request is denied?
Don’t panic! First, carefully review your Explanation of Benefits (EOB) to find the specific denial code. If the denial was due to a simple clerical error, you can often fix it and resubmit. If you disagree with the decision, you have the right to initiate a formal appeals process by providing additional clinical notes or a letter of medical necessity from your doctor.
Is it necessary to keep copies of my forms after I have submitted them?
Absolutely. It is a best practice to keep digital copies or photocopies of every document you send to your insurance company. Having a record of your claim reference number and all attachments will be invaluable if you need to speak with a customer service representative regarding a delay or dispute.